Hair Regeneration with Stem Cell Therapy: Clinical Evidence, Regenerative Mechanisms & Asia Access 2025
Estimated Reading Time: 15-18 minutes
Table of Contents
Understanding Hair Loss and Follicle Biology
Hair loss, or alopecia, can result from a variety of causes — ranging from genetics and hormonal factors to immune reactions, stress, and medical treatments. The two most common types are androgenetic alopecia (pattern baldness) and alopecia areata (spot baldness), each involving different biological mechanisms but sharing a common outcome: the disruption of normal hair follicle activity.
Androgenetic Alopecia (Pattern Baldness)
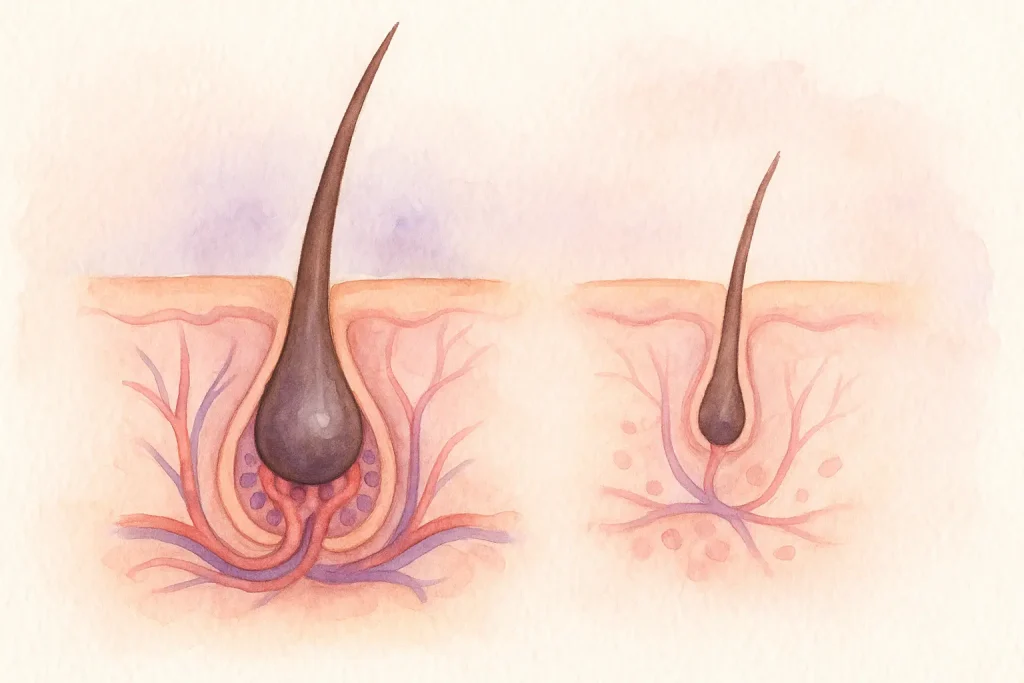
This form of hair loss is primarily hereditary and linked to hormonal sensitivity. It is characterized by gradual follicular miniaturization — a process in which hair follicles shrink and produce thinner, shorter hairs over time. Sensitivity to dihydrotestosterone (DHT), a hormone derived from testosterone, plays a major role in this process. In men, this typically presents as a receding hairline or crown thinning, while in women it appears as diffuse thinning over the top of the scalp.
Alopecia Areata (Spot Baldness)
Alopecia areata is an autoimmune disorder in which the immune system mistakenly attacks the hair follicles, leading to patchy, round areas of hair loss on the scalp or body. It can sometimes progress to total scalp hair loss (alopecia totalis) or complete body hair loss (alopecia universalis). The condition can appear at any age and often follows an unpredictable course — some cases resolve spontaneously, while others persist or recur.
The Hair Growth Cycle
Each hair follicle follows a repeating cycle of growth, transition, and rest. The three main phases are summarized below.
Anagen (Growth Phase)
Duration: 2–7 years
Active growth phase in which most scalp hairs remain in a prolonged regenerative state.
Catagen (Transition Phase)
Duration: 2–3 weeks
The follicle shrinks, detaches from the dermal papilla, and prepares to transition to rest.
Telogen (Resting Phase)
Duration: 2–4 months
The follicle rests before shedding old hair and returning to a new anagen cycle.
In androgenetic alopecia, the anagen phase shortens while the telogen phase lengthens, leading to thinner, weaker hair strands. In alopecia areata, immune activity disrupts this cycle, forcing follicles prematurely into rest and shedding phases.
Biology of the Hair Follicle
At the cellular level, hair follicles are mini-organs capable of continuous self-renewal. Key cells such as dermal papilla cells (DPCs) — located at the base of each follicle and responsible for signaling hair growth — and outer root sheath cells regulate follicular activity through signaling pathways including Wnt/β-catenin, BMP, and TGF-β, all of which are key regulators identified in current regenerative biology research. When inflammation, oxidative stress, or hormonal imbalance disrupt these molecular pathways, follicles lose their regenerative capacity and gradually enter dormancy. This breakdown of communication within the follicle’s microenvironment is a central factor in chronic or progressive hair loss.Why This Matters
Understanding the biology behind hair growth provides insight into why traditional therapies — such as topical or oral medications — often provide only temporary improvement. Stem cell–based treatments aim to restore lost signaling communication, rejuvenate follicular stem cells, and promote angiogenesis, thereby supporting long-term regeneration rather than short-term stimulation.
How Stem Cell Therapy Works for Hair Regeneration
Stem cell-based therapy for hair restoration focuses on repairing and rejuvenating the follicular microenvironment — the biological niche that supports continuous hair growth. By reactivating dormant follicles, regulating inflammation, and promoting angiogenesis (new blood vessel formation), this approach addresses the underlying causes of progressive hair thinning rather than merely masking its appearance.
Types of Stem Cells and Regenerative Biologics
Stem cell-based treatments for hair restoration involve several biologically distinct cell types and regenerative components, each contributing differently to follicular repair and growth.
Mesenchymal Stem Cells (MSCs)
The most widely studied and clinically used stem cells for hair regeneration, capable of repairing tissue and modulating inflammation through paracrine signaling. They can be derived from multiple tissue sources:
- Adipose-derived MSCs (AD-MSCs): Obtained from the patient’s own fat tissue; rich in growth factors and cytokines that stimulate follicle recovery.
- Bone marrow-derived MSCs (BM-MSCs): Multipotent cells with regenerative and immunomodulatory functions.
- Umbilical cord–derived MSCs (UC-MSCs): Allogeneic cells from healthy donors; known for high immune compatibility and potent regenerative signaling.
MSCs act primarily by releasing growth factors that regulate inflammation, enhance microcirculation, and stimulate local follicular stem cells.
Hair Follicle Stem Cells (HFSCs)
Located in the bulge region of each follicle, HFSCs drive natural hair renewal throughout every growth cycle. Current research focuses on methods to reactivate or expand HFSC populations to restore lost follicles in both androgenetic alopecia and alopecia areata.
Platelet-Rich Plasma (PRP)
PRP is a concentrated preparation of the patient’s own blood containing growth factors such as VEGF, PDGF, and IGF-1, which improve blood flow and stimulate follicular activity. While not technically a stem cell therapy, PRP plays a complementary role by enhancing scalp healing and supporting active follicles.
Mechanisms of Action
Stem cells and regenerative biologics promote hair growth through several complementary biological effects:
1. Growth Factor Secretion
Key signaling molecules include:
- VEGF (Vascular Endothelial Growth Factor): Promotes blood vessel formation and nutrient delivery.
- FGF (Fibroblast Growth Factor): Stimulates follicle cell proliferation and prolongs the anagen (growth) phase.
- IGF-1 (Insulin-like Growth Factor 1): Supports hair shaft elongation and follicle survival.
- HGF (Hepatocyte Growth Factor): helps transition follicles from resting (telogen) to growth (anagen) phases.
2. Follicle Activation and Proliferation
Stem cells awaken dormant follicles, stimulate dermal papilla cells (specialized cells at the follicle base that regulate growth signals), and increase the proliferation of matrix cells that form new hair shafts.
3. Angiogenesis and Collagen Remodeling
Regenerative biologics improve microcirculation, promote new capillary formation, and support collagen remodeling — creating a healthier, oxygen-rich environment for follicle regrowth.
4. Anti-Inflammatory and Immunomodulatory Effects
MSCs reduce scalp inflammation by suppressing pro-inflammatory cytokines such as TNF-α and IL-6.
In autoimmune conditions like alopecia areata, they help rebalance immune activity and protect follicles from immune-mediated damage.
5. Prolongation of the Anagen Phase
Stem cell secretions extend the duration of active hair growth, resulting in thicker, longer hair strands before entering the resting phase.
6. Reversal of Miniaturization
By restoring follicular signaling and tissue integrity, MSC therapy may enlarge miniaturized follicles — a hallmark of androgenetic alopecia — and potentially slow or reverse the miniaturization process.
Clinical Evidence: What Research Shows
Safety Profile
- Clinical studies consistently demonstrate that stem cell and PRP–based hair restoration therapies have a favorable safety profile when performed by trained professionals under sterile conditions.
- Most side effects are mild and temporary, such as slight redness or swelling at the injection site.
- A recent Dermatologic Therapy review (2022) reported no serious adverse events across trials using adipose-, bone marrow–, or umbilical cord–derived MSCs, while Stem Cells Translational Medicine also confirmed strong biocompatibility and minimal immune reaction in repeated applications.
- Long-term data remain limited but follow-ups up to three years indicate sustained safety.
Efficacy Findings
Androgenetic Alopecia (Pattern Baldness)
Recent clinical and meta-analytic research supports measurable improvements in hair density, thickness, and patient satisfaction following MSC- and PRP-based treatments for androgenetic alopecia (AGA).
- Platelet-Rich Plasma (PRP): A 2020 systematic review reported that PRP significantly increased hair density and patient satisfaction compared with placebo or minoxidil controls, although study heterogeneity remains high. [Int J Mol Sci . 2020 – PubMed]
- Adipose-Derived Stem Cell Constituent Extract (ADSC-CE): A double-blind, vehicle-controlled clinical trial demonstrated statistically significant improvement in both hair count and thickness after 16 weeks of topical ADSC-CE application, confirming efficacy with excellent safety and tolerance. [J Cutan Aesthet Surg. 2021 – PMC]
- Combined MSC + PRP Regenerative Approach: A 2025 study using stromal vascular fraction (SVF)-enhanced PRP reported increased hair density and scalp coverage in patients with AGA, suggesting potential synergy between cellular and platelet-based regenerative modalities. [Stem Cell Research & Therapy, in press]
Current evidence indicates that PRP and certain MSC-derived biologics (such as ADSC-CE and SVF-enriched PRP)can improve hair density, thickness, and patient satisfaction with good tolerability.
However, treatment protocols vary widely across studies, and larger, standardized, long-term randomized controlled trials are needed to confirm efficacy and durability of results.
Alopecia Areata (Autoimmune Hair Loss)
Emerging research suggests that MSC-based therapy may provide benefits in alopecia areata by modulating immune activity and promoting hair follicle recovery. For example, a 2024 pilot study observed hair regrowth and reduced inflammatory markers following local MSC application in AA. Int J Mol Sci . 2024 – PubMed.
Meanwhile, PRP has been evaluated in a 2022 systematic review and found to be a potential steroid-free option, though the quality of evidence remains limited and responses are variable. [Biomedicines, 2022 – MDPI]
These findings are promising, but both MSC and PRP treatments for AA remain investigational, and larger randomized controlled trials are required before routine use.
Combination and Comparative Studies
- Combination approaches integrating mesenchymal stem cells (MSCs) with platelet-rich plasma (PRP) have demonstrated superior clinical outcomes — including faster improvement, enhanced follicle survival, and improved graft recovery — compared with PRP alone. These synergistic effects are attributed to complementary growth-factor signaling between stem- and platelet-derived cytokines. [Regenerative Therapy, 2022] [Cells, 2019]
- Comparative trials indicate that MSC-based treatments can achieve equal or greater gains in hair density than topical minoxidil, with longer-lasting effects following treatment completion. [Stem Cell Research & Therapy, 2023]
Longevity of Effect
Current research supports short- to mid-term safety and efficacy for stem cell–based hair restoration, though long-term durability is still being defined. The insights below summarize consistent findings across published clinical studies.
Small Sample Sizes
Most studies enroll 10–50 participants, limiting statistical power and overall generalizability.
Short Follow-Up Duration
Most clinical trials track outcomes for only 6–24 months; few extend beyond 3 years.
Variable Treatment Protocols
Differences in cell source, dosage, concentration, and session frequency make comparisons difficult.
Inconsistent Response Rates
Approximately 60–70% of patients show visible improvement, while others report modest or minimal change.
Need for Standardization
Experts highlight the importance of multi-center randomized trials to establish optimal dosing, intervals, and long-term maintenance.
Emerging Consensus
Systematic reviews show consistent short-term gains in density and thickness, but evidence beyond 2–3 years is still limited.
Overall, stem cell–based hair restoration shows encouraging short- to mid-term results, but true long-term durability remains under active investigation.
Comparison with Existing Treatments
Below is a comparison of conventional therapies and regenerative approaches, highlighting differences in mechanisms, limitations, and expected duration of effect.
Main Mechanism: Improves scalp blood flow
Limitation: Requires continuous use
Duration: Temporary
Main Mechanism: Suppresses DHT production
Limitation: Hormonal side effects; male-only
Duration: Continuous
Main Mechanism: Platelet-derived growth factors
Limitation: Short duration; variable efficacy
Duration: 6–12 months
Main Mechanism: Surgical follicle relocation
Limitation: Donor availability; recovery time
Duration: Permanent (transplanted hairs)
Main Mechanism: Regenerates follicular microenvironment; modulates immunity
Limitation: Experimental; requires multiple sessions
Duration: 12–18 months potential
Access and Regulation in Asia
Regulatory Context
- Japan: Under the Act on the Safety of Regenerative Medicine, most private-clinic MSC procedures use autologous cells, with allogeneic MSCs limited to specific approved products or clinical trials.
- South Korea: Hospital-based MSC therapies are mainly autologous, and the use of allogeneic MSC products is tightly controlled under regenerative medicine regulations.
- Malaysia: Under MOH stem cell / CGTP guidelines, licensed centers can clinically use cultured allogeneic MSCs—including Wharton’s jelly–derived WJ-MSCs—within a government-led, guideline-driven framework.
- Singapore & Thailand: MSC therapies are regulated as cell/tissue/gene therapy products in accredited centers, with access to allogeneic cultured MSCs generally limited to registered products or formal studies rather than broad medical-tourism offerings.
Within this group, Malaysia is one of the countries where allogeneic cultured MSCs such as WJ-MSCs are available to patients under clear national guidelines.
Access and Clinical Practice
Treatments are typically administered in specialized regenerative or dermatology clinics. MSC preparations are delivered via microinjection or infusion, often in outpatient settings. Pre-treatment evaluation includes scalp imaging and blood screening to ensure safety and candidacy.
Insurance and Cost
Most Asian insurers classify MSC therapy as investigational. Patients generally pay out-of-pocket, though premium or international health plans may offer partial reimbursement. Costs vary by cell source and number of sessions, with Malaysia and Thailand providing more accessible pricing compared to Japan or Korea.
Benefits and Limitations
Stem cell–based hair restoration offers regenerative advantages but also presents clinical and practical limitations. The overview below provides a balanced, evidence-based summary to support informed decision-making.
Potential Benefits
- Non-surgical and minimally invasive procedure
- Stimulates natural follicular regeneration & scalp rejuvenation
- May improve density, thickness, and overall hair quality
- Minimal downtime; compatible with PRP or low-level laser therapies
- Does not affect systemic hormone levels (unlike finasteride)
Key Limitations
- Clinical evidence is still evolving; outcomes vary by individual
- Ineffective in areas where no viable follicles remain
- Periodic maintenance may be required for sustained results
- Cost, accessibility & regulatory pathways differ across Asia
The Future of Stem Cell Hair Restoration
Next-generation regenerative approaches are rapidly emerging in hair science and clinical dermatology:
- Exosome-based therapy: Utilizes cell-free vesicles enriched with growth factors, cytokines, and RNA molecules that signal follicular regeneration.
- 3D follicle organoid research: Focuses on recreating functional mini-follicles from stem cells under laboratory conditions, aiming to enable de novo hair follicle formation.
- Gene-edited MSCs: Engineered to enhance Wnt/β-catenin pathway activation, potentially improving follicular growth and longevity.
- Synergistic combination protocols: Integrate MSCs with platelet-rich plasma (PRP), microneedling, or low-level laser therapy to maximize scalp rejuvenation and hair density outcomes.
Together, these innovations mark a transition from experimental interventions toward structured, evidence-based regenerative dermatology across Asia.
Frequently Asked Questions (FAQ)
Below are evidence-informed answers to common questions about stem cell–based hair
regeneration, including candidacy, safety, and how protocols differ across Asia.
Malaysia regulates regenerative medicine under the National Cell and Gene Therapy Guidelines (2021). Licensed clinics may offer MSC-based treatments for dermatological use within clinical protocols, but therapies remain investigational rather than fully approved.
Most studies report visible improvement lasting 12–18 months. Maintenance sessions may be needed every 9–12 months to sustain follicular stimulation.
Ideal candidates have partial hair thinning with viable follicles—commonly early- to mid-stage androgenetic alopecia or autoimmune-related patch loss. Complete baldness (no active follicles) responds poorly.
Yes. Combining MSCs and PRP can produce faster, more sustained regrowth due to complementary growth-factor signaling and improved scalp healing.
Most patients experience only mild redness or swelling for 1–3 days and resume normal activity immediately.
Reported effects are minor—temporary tenderness or scalp warmth. Serious complications are rare when performed in sterile, accredited facilities.
Clinical protocols differ slightly by country. Japan and South Korea follow strict regenerative-medicine frameworks, while Malaysia and Thailand provide access through licensed cell-therapy programs. Always verify that your clinic is accredited before treatment.
Absolutely. MSC and PRP therapies have shown efficacy in female-pattern hair thinning, particularly post-menopausal or stress-related cases.
Current evidence shows sustained benefits up to 18-24 months. Long-term permanence is still under clinical study.
Conclusion
Stem cell therapy represents a biologically restorative approach to hair loss management—targeting the regeneration of follicular structures rather than temporary surface stimulation.
Early clinical findings indicate measurable improvements in hair density, scalp condition, and patient-reported satisfaction, supported by an overall favorable safety profile.
Nevertheless, stem cell–based hair restoration remains an emerging field. Patients are advised to consult qualified regenerative medicine specialists, verify clinic accreditation and treatment protocols, and maintain realistic expectations regarding outcomes.
As scientific understanding and clinical standardization progress, MSC-driven regenerative therapies may soon become an integral component of comprehensive hair restoration strategies across Asia. Individuals who wish to understand whether regenerative approaches may be appropriate for their condition may speak with a licensed specialist or contact us for further guidance.
Scientific References
- Dermatologic Therapy (2022). Safety review of adipose-, bone marrow–, and umbilical cord–derived MSCs in dermatology. PubMed 35948034
- Stem Cells Translational Medicine. Biocompatibility and immune tolerance of repeated MSC applications. PubMed 30723013
- International Journal of Molecular Sciences (2020). Systematic review of PRP efficacy for androgenetic alopecia. PubMed 32295047
- Journal of Cutaneous and Aesthetic Surgery (2021). ADSC-CE double-blind clinical trial for hair density improvement. PMC 8611710
- Stem Cell Research & Therapy (2025, in press). Stromal vascular fraction (SVF)–enhanced PRP for androgenetic alopecia. 10.1186/s13287-025-04560-7
- International Journal of Molecular Sciences (2024). MSC pilot study for alopecia areata and immunomodulation. PubMed 39273184
- Biomedicines (2022). Systematic review of PRP as a steroid-free option for alopecia areata. Biomedicines 2022;10(8):1829
- Regenerative Therapy (2022). MSC + PRP combination therapy improving graft survival and clinical recovery. S2352-3204(22)00102-X
- Cells (2019). Clinical outcomes of MSC and platelet-derived product synergy in hair restoration. PubMed 31100937
- Stem Cell Research & Therapy (2023). Systematic review on MSC-based therapies for hair loss and long-term outcomes. 10.1186/s13287-023-03440-2
ℹ Disclaimer
This article is intended for informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment recommendation. Stem cell therapy for hair loss is an emerging field, with ongoing research into optimal protocols, long-term safety, and clinical efficacy. Treatment availability, legal status, and clinical standards vary by country and institution. Individual outcomes depend on patient-specific factors and cannot be guaranteed.
Always consult licensed healthcare professionals—including dermatologists and specialists in regenerative medicine—before making any treatment decisions. The information provided reflects current knowledge from peer-reviewed scientific sources and clinical practice as of November 2025, and may evolve as new research emerges. As scientific understanding and clinical standardization progress, MSC-driven regenerative therapies may soon become an integral component of comprehensive hair restoration strategies across Asia.
Last Updated: November 2025