Stem Cell Therapy for Dental Regeneration: A Comprehensive Guide 2025
Estimated Reading Time: 10-12 minutes
Table of Contents
Introduction
Tooth loss and damage to dental tissues have long been regarded as unavoidable outcomes of disease, trauma, or aging. Conventional dental treatments, such as fillings, root canals, and implants, are effective in restoring form and function but cannot truly regenerate living tissue.
In recent years, advances in regenerative medicine have introduced a new possibility: using stem cells to repair and restore the tooth’s own biological structures. Rather than replacing what is lost, this approach seeks to revive natural vitality, circulation, and defense mechanisms within the tooth. Stem cell-based dental therapies are at the forefront of this transformation. From revitalizing dental pulp after root canal procedures to reconstructing periodontal tissue damaged by gum disease, these treatments are reshaping how dentistry approaches healing.
This guide provides a comprehensive overview of current clinical evidence, ongoing research, and real-world applications across Asia, where some of the world’s most advanced regenerative dental studies are taking place.

What Is Dental Stem Cell Therapy?
Dental stem cell therapy uses specialized cells, primarily dental pulp stem cells (DPSCs), to repair or regenerate damaged dental tissues. These cells can be harvested from:
- Dental pulp (the soft tissue inside teeth)
- Periodontal ligament (tissue connecting teeth to bone)
- Apical papilla (tissue at the developing root tip)
- Gingival tissue (gum tissue)
- Exfoliated deciduous teeth (baby teeth, known as SHED cells)
Unlike embryonic stem cells, dental stem cells raise minimal ethical concerns and are relatively easy to obtain, often from extracted wisdom teeth or baby teeth that naturally fall out.
How It Works
When introduced into damaged dental tissue, stem cells don’t necessarily transform directly into new teeth or pulp. Instead, they work through several key mechanisms:
- Paracrine signaling: Release growth factors that promote healing and regeneration
- Cell differentiation: Transform into odontoblasts (dentin-forming cells) or other specialized dental cells
- Anti-inflammatory effects: Reduce tissue inflammation and create a healing environment
- Angiogenesis: Stimulate new blood vessel formation to restore blood supply
Current Clinical Applications
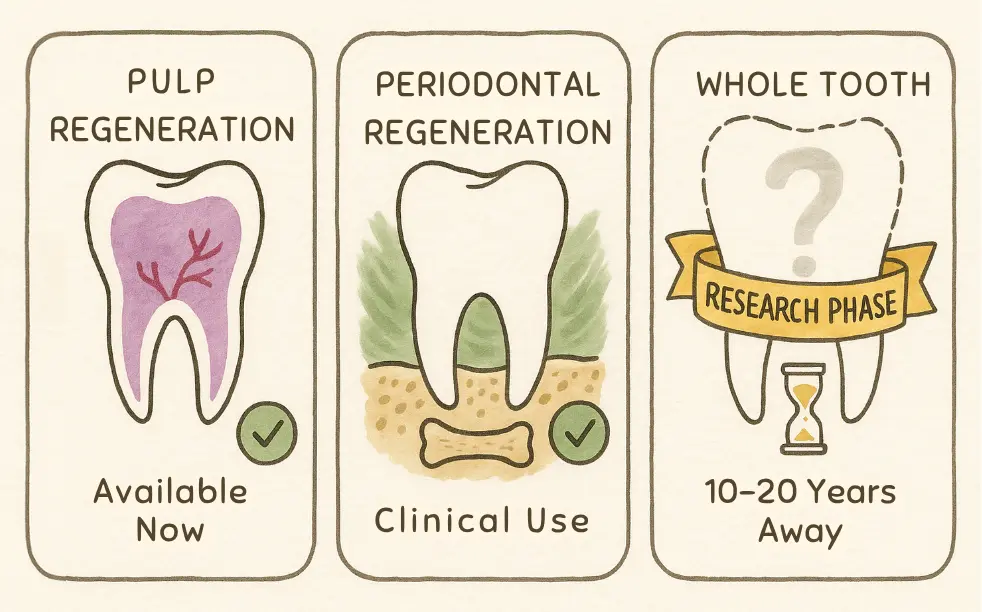
1. Dental Pulp Regeneration (Endodontic Regeneration)
The Challenge: Traditional root canal treatment removes infected pulp tissue, leaving the tooth “dead”, without sensation, blood supply, or natural defense mechanisms.
The Solution: Stem cell therapy aims to regenerate functional pulp tissue, potentially allowing treated teeth to remain vital.
Clinical Evidence:
- A pilot clinical study in Japan demonstrated that autologous dental pulp stem cells (DPSCs) transplanted into pulpectomized teeth restored vitality, showing positive electric pulp test (EPT) responses within four weeks and MRI evidence of pulp-like tissue formation (Stem Cell Research & Therapy, PubMed).
- Autologous stem cells from exfoliated deciduous teeth (SHED) successfully regenerated necrotic dental pulp when implanted into injured immature permanent teeth, forming vascularized and innervated pulp-like tissue(Science Translational Medicine, DOI: 10.1126/scitranslmed.aaf3227).
- A prospective randomized controlled trial involving 40 patients (30 treated + 10 controls) using SHED-based therapy achieved revascularization, sensory response to electric stimulus, and increased root length at 12 months, with no adverse events reported during follow-up, some patients were monitored for up to 24 months for safety (World Journal of Stem Cells, Clinical trials using dental stem cells: 2022 update).
Current Status: Several clinical trials are underway, particularly in Japan and China, but pulp regeneration remains experimental. These procedures require specialized GMP-compliant facilities and are not yet standard care.
2. Periodontal Tissue Regeneration
The Challenge: Periodontal disease destroys the supporting structures of teeth, gums, ligaments, and bone, leading to tooth loss. Conventional treatments can halt progression but struggle to regenerate lost periodontal tissue.
The Solution: Stem cell therapy seeks to restore these supporting tissues by injecting or transplanting regenerative cells capable of rebuilding the periodontal ligament, alveolar bone, and gingival tissue.
Clinical Evidence:
- A multicenter randomized clinical trial in China with 132 patients suffering from chronic periodontitis demonstrated that dental pulp stem cell (DPSC) injections resulted in significant improvement in bone defect depth (0.30 mm vs 0.04 mm with saline) and clinical attachment level. The greatest benefit was observed in Stage III periodontitis patients (Signal Transduction and Targeted Therapy, PubMed).
- A randomized controlled clinical trial using autologous DPSC micrografts combined with a collagen sponge scaffold showed significantly greater probing-depth reduction, clinical attachment gain, and bone fill compared with collagen alone after 12 months (Journal of Clinical Periodontology, PubMed).
- A pilot clinical study involving 15 patients with avulsed teeth showed that transplantation of deciduous dental pulp stem-cell (hDPSC) aggregates within a bioengineered microenvironment promoted functional periodontal regeneration and continued root development during follow-up (Biomaterials, PubMed).
Current Status:
Periodontal regeneration using stem cells is further advanced than pulp regeneration, with several human studies demonstrating measurable structural and clinical improvements. However, protocols remain unstandardized, and most applications are still confined to research or specialized regenerative centers, particularly in Asia.
3. Whole Tooth Regeneration (Experimental)
The Ultimate Goal: Growing an entirely new biological tooth to replace a lost one.
Current Reality: While scientists have successfully grown tooth-like structures in laboratory animals, complete human tooth regeneration remains purely experimental and is not yet available clinically.
Research Progress:
- Studies have demonstrated tooth bud formation in mice.
- Bioengineered tooth constructs using stem cells combined with scaffolds show promise.
- Major technical challenges include:
- Creating properly shaped teeth
- Ensuring correct positioning and integration
- Achieving functional enamel formation
- Establishing neurovascular connections
Current Status:
Most experts estimate that clinical availability is still 10-20 years away at minimum. Current focus remains on tissue-specific regeneration (pulp, periodontium) rather than whole-tooth replacement.
Clinical Evidence: What Research Shows
Safety Profile
Clinical evaluations of mobilized dental pulp stem cell (MDPSC) transplantation have demonstrated no adverse events or toxicity in treated patients. Multiple studies across dental applications report:
- Low complication rates: Minimal side effects, typically limited to mild temporary discomfort
- No serious adverse events: No reports of tumor formation, immune rejection, or severe reactions
- Good tolerability: Most patients undergo the procedure without significant complications.
For example, a pilot human study using autologous MDPSCs in pulpectomized teeth reported no serious side effects and successful pulp-like tissue formation (Stem Cell Research & Therapy, PubMed).
Efficacy Findings
A systematic review published in 2024 examining the therapeutic use of dental mesenchymal stem cells in human clinical trials found widespread interest and significant potential for their use in dental pulp regeneration, periodontal repair, and even systemic disease therapies, highlighting encouraging short-term safety and efficacy outcomes but noting that long-term evidence and standardized clinical protocols remain limited (Journal of Dental Research, DOI: 10.1177/00220345241261900).
Key outcomes observed:
- Pulp regeneration: Restoration of pulp-like tissue with neovascularization (Tissue Engineering & Regenerative Medicine, PubMed / DOI: 10.1007/s13770-021-00389-2).
- Periodontal improvement: Measurable gains in attachment levels and bone depth observed in a multicenter RCT using DPSC injection for chronic periodontitis (Signal Transduction and Targeted Therapy, PubMed).
- Tooth sensitivity: Recovery of sensation in previously non-vital teeth, as reported in small pilot studies using autologous pulp stem cells (Stem Cell Research & Therapy, PubMed).
- Root development: Continued root growth observed in immature permanent teeth following SHED-based transplantation (Science Translational Medicine, DOI: 10.1126/scitranslmed.aaf3227).
Important Limitations
Despite these encouraging findings, researchers emphasize that clear long-term cost-benefit evidence and proof of improved tooth retention beyond conventional treatments remain limited.
- Most clinical studies involve small sample sizes (5-50 patients) and short-term follow-up (International Journal of Molecular Sciences, DOI: 10.3390/ijms22094357).
- Long-term data (5-10 years) are still lacking.
- Protocols vary across studies, making comparisons difficult.
- Outcomes differ by patient age, disease severity, and systemic health status.
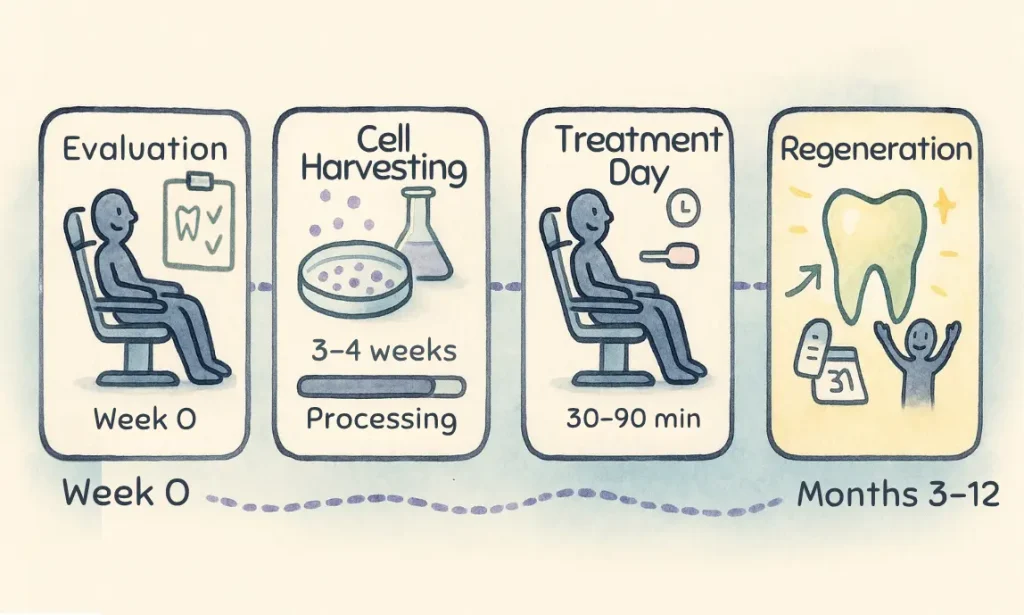
The Treatment Process
Pre-Treatment Evaluation
Patients typically undergo:
- Comprehensive dental examination
- Radiographic imaging (X-rays, CBCT, possibly MRI)
- Assessment of tooth viability and disease severity
- Medical history review
- Discussion of expectations and alternatives
Cell Collection
For Autologous Treatment (using patient’s own cells)
- Extraction of wisdom tooth or other suitable tooth
- Pulp tissue harvested under sterile conditions
- Cells isolated and expanded in GMP-certified laboratory
- Process typically takes 3-4 weeks
For Allogeneic Treatment (using donor cells)
- Pre-processed stem cells from tissue banks
- Derived from donated umbilical cords, baby teeth, or adult dental tissue
- Quality-tested and ready for immediate use
Administration
Depending on the condition:
- Pulp regeneration: Cells placed directly into cleaned root canal with scaffold material
- Periodontal regeneration: Injection into affected gum tissue or surgical placement with membrane
- Procedures typically performed under local anesthesia
- Treatment time: 30-90 minutes
Post-Treatment Care
- Regular follow-up appointments
- Imaging to assess tissue regeneration
- Monitoring for complications
- Standard dental hygiene maintained
- Results typically assessed over 6-12 months
Availability Across Asia
Dental stem cell therapy availability varies across countries in Asia, reflecting different stages of research, regulation, and clinical adoption.
Countries Offering Clinical Treatment:
- Japan: Leading in pulp regeneration research and early clinical applications.
- China: Multiple centers offering periodontal regeneration using dental stem cells.
- South Korea: Advanced research infrastructure with selected clinical offerings.
- Thailand: Emerging hub for dental tourism incorporating regenerative treatments.
- Singapore: Primarily research-focused, with limited but well-regulated pilot applications.
- Malaysia: Growing interest in regenerative dentistry; clinical use currently limited to research and feasibility programs.
Regulatory Considerations
Treatment standards and approval pathways differ by country. Patients should verify:
- National health authority oversight (e.g., Ministry of Health Malaysia, FDA, PMDA in Japan)
- GMP-certified cell processing and handling facilities
- Licensed dental specialists with regenerative medicine training
- Transparent protocols, patient consent, and follow-up procedures
Benefits, Risks, and Limitations
Potential Benefits
Biological restoration
- Preserves tooth vitality rather than creating “dead” teeth
- Potential for natural healing and continued development
- Restores sensation and defense mechanisms
Minimally invasive
- Often less invasive than traditional surgery
- Faster recovery compared to some conventional procedures
- Potential to avoid tooth extraction
Long-term promise
- May reduce need for future interventions
- Biological integration with existing structures
- Potential for continued improvement over time
Risks and Side Effects
Common (mild)
- Temporary discomfort or sensitivity
- Minor swelling at treatment site
- Transient inflammation
Rare but possible
- Infection (if sterile protocols not followed)
- No therapeutic response (20-40% of patients in some studies)
- Unpredictable outcomes
Unknown
- Very long-term safety (>10 years) not yet established
- Potential for unexpected tissue responses
Important Limitations
Clinical limitations
- Not a guaranteed solution
- Cannot address all dental problems
- May require multiple treatments
- Success depends on remaining tissue health
Practical limitations
- Limited availability outside major research centers
- High cost without insurance coverage
- Requires specialized facilities and expertise
- Long processing times for autologous cells
Scientific limitations
- Optimal protocols still being refined
- Best cell types, dosages, and delivery methods unclear
- Individual response unpredictable
Who Might Be a Candidate?
Dental stem cell therapy may be suitable for:
Good Candidates
- Patients with necrotic pulp but otherwise healthy teeth
- Individuals with moderate periodontal disease
- Those seeking to preserve natural teeth
- Patients with immature permanent teeth requiring treatment
- Individuals who have suitable teeth for cell harvesting
- People willing to accept experimental nature and follow-up requirements
Not Recommended For
- Severe tooth structural damage beyond repair
- Advanced periodontal disease with extensive bone loss
- Active oral infection (must be controlled first)
- Patients with certain systemic diseases affecting healing
- Those unable to maintain adequate oral hygiene
- Individuals expecting guaranteed results
- Patients seeking immediate solutions (regeneration takes months)
The Future: What’s on the Horizon?
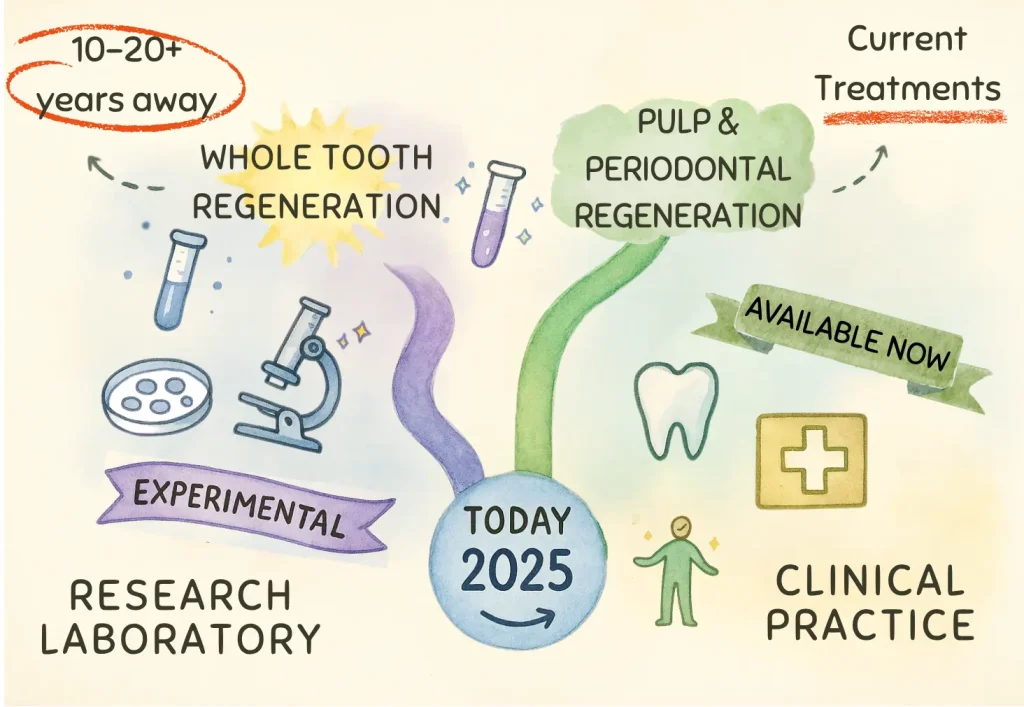
Emerging Technologies
Tissue Engineering Advances
- 3D-bioprinted scaffolds mimicking natural tooth structure
- Smart biomaterials that release growth factors on demand
- Gene-enhanced stem cells with improved regenerative capacity
Improved Cell Therapies
- Cell-free therapies using exosomes (cell-derived vesicles)
- Combination treatments with growth factors and biomaterials
- Standardized, off-the-shelf stem cell products
Whole Tooth Regeneration
- Continued research into bioengineered tooth organs
- Investigation of tooth bud transplantation techniques
- Long-term goal of replacing implants with biological teeth
Realistic Expectations
While research is promising, patients should understand:
- Whole tooth regeneration remains experimental and likely decades away from clinical use
- Current applications focus on specific tissue regeneration, not complete tooth replacement
- Technology continues evolving, but regulatory approval takes time
- Today’s experimental treatments may become tomorrow’s standards, but this process is gradual
Frequently Asked Questions (FAQ)
Q1: Can stem cells grow me a whole new tooth?
Not yet. Whole tooth regeneration is experimental and years away from clinical use.
Q2: Is dental stem cell therapy safe?
Clinical studies show good safety profiles with minimal adverse events. However, long-term data (beyond 5-10 years) are still limited. Treatment should only be performed in regulated facilities with proper oversight.
Q3: How long until I see results?
Tissue regeneration is gradual. Initial signs may appear within weeks, but meaningful regeneration typically takes 3-6 months, with continued improvement possible up to 12-24 months.
Q4: Will my insurance cover this?
Most insurance plans currently classify dental stem cell therapy as experimental and do not provide coverage. Patients typically pay out-of-pocket.
Q5: Where can I get dental stem cell treatment?
Availability varies by country and procedure type. Japan, China, and South Korea have the most clinical experience. Always verify facility credentials and regulatory compliance.
Q6: Can I bank my child’s baby teeth for future use?
Yes. Several companies offer dental stem cell banking services, storing cells from baby teeth for potential future use. Annual storage fees apply.
Q7: How does this compare to dental implants?
Implants are proven, reliable replacements for missing teeth. Stem cell therapy aims to save or regenerate natural tissue rather than replace it. They serve different purposes and are not direct alternatives.
Q8: What’s the success rate?
Success varies by procedure and patient. Published studies show positive outcomes in 60-80% of cases for pulp regeneration, with higher success rates for periodontal applications. Individual results vary significantly.
Conclusion
Stem cell therapy represents an exciting frontier in dental medicine, one that offers the promising possibility of biological repair rather than mechanical replacement. The evidence from clinical trials across Asia and globally shows measurable benefits for specific applications, particularly dental pulp and periodontal regeneration.
However, it’s crucial to maintain realistic expectations. This is not yet a mainstream treatment, and whole tooth regeneration remains a distant goal.
For patients considering dental stem cell therapy:
- Consult with qualified dental specialists experienced in regenerative dentistry
- Verify clinic credentials and ensure compliance with national health regulations
- Understand the experimental nature of current treatments
- Consider conventional proven treatments as primary options
- View stem cell therapy as a potential adjunct or alternative when appropriate
As research continues and technology advances, stem cell-based approaches will likely become more refined, accessible, and effective. While we’re not yet at the point of growing replacement teeth on demand, we’re witnessing the early stages of a transformation in how dental disease and damage can be treated.
For more information about regenerative dental treatments or to explore whether emerging stem cell therapies might be appropriate for your dental health needs, consult with qualified dental professionals and stay informed about ongoing research developments.
ℹ Disclaimer
This article is intended for informational and educational purposes only and does not constitute medical or dental advice. Stem cell-based dental treatments remain largely experimental, with ongoing research into their safety, efficacy, and regulatory approval. Availability, legal status, and treatment standards vary by country and institution. Individual outcomes depend on patient-specific factors and cannot be guaranteed. Always consult licensed dental or medical professionals before considering any treatment.
Last Updated: October 2025